Friends and countrymen, today we will start a journey down the road of convalescent care in grid down and covert environs. The trip won’t be short, because there are many aspects to cover, and we will try to get in as much as we can without putting people to sleep. We anticipate that we may have some lively commentary where hopefully some folks who do some of this work can chime in and enlighten us.
To be merciful to you, the readers, and ourselves, the guys who have to write this stuff, we will do this as a series of posts so that we can focus on certain areas and not write an entire textbook in one post.
First, let’s define convalescent via Webster’s.
convalescent
Medical Definition of CONVALESCENT
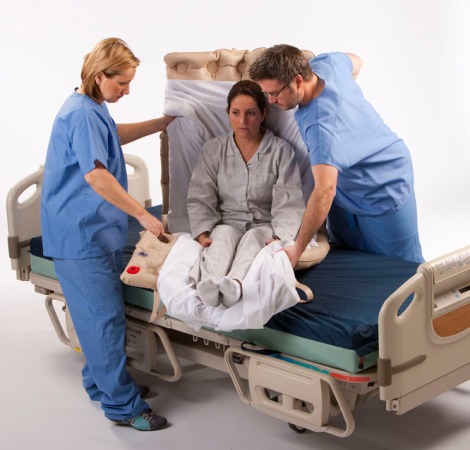
You’ve just splinted your buddy’s broken femur and decompressed his left chest after a fall while rock climbing.Now what?Transport him out ASAP and get him to surgery.OK, they have screws in his femur with a big old cast and his chest is all sewn up.Now what?He’s got to heal. And he’s going to need a clean room, a bed, sheets, bandages, pain medication, antibiotics, food, bathroom help, baths, and routine checkups from the doc and nurses to assess his progress.
Real talk
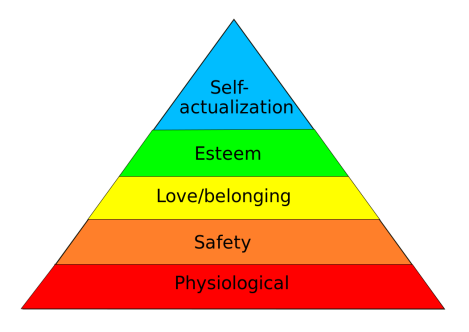
Physiological needs
Physiological needs are the physical requirements for human survival. Physiological needs are thought to be the most important; they should be met first. Air, water, and food are metabolic requirements for survival in all animals, including humans. Clothing and shelter provide necessary protection from the elements.[2] In a medical context, this may include the needed medications and treatment to keep your buddy alive, such as insulin for a diabetic, etc.
Safety needs
With their physical needs relatively satisfied, the individual’s safety needs take precedence and dominate behavior.
Safety and Security needs include:
- Personal security–protect your grid-down mates from either the charging bear, flash floods, or the rampaging zombie horde
- Financial security–who will take care of your buddy’s wife & kids while he is out of commission?
- Health–applies medically in terms of clean or sterile materials, protection from infection, getting the right treatment to the right patient, & etc.
Where we may quibble with Maslow’s Hierarchy for grid down convalescent care is to swap the two bottom needs so that Safety is the base and Physiological is one step above, or they are blended together as one.
Love and belonging
After physiological and safety needs are fulfilled, the third level of human needs is interpersonal and involves feelings of belongingness. This need is especially strong in childhood and can override the need for safety as witnessed in children who cling to abusive parents. Deficiencies within this level of Maslow’s hierarchy – due to hospitalism, neglect, shunning, ostracism, etc. – can impact the individual’s ability to form and maintain emotionally significant relationships in general, such as:
- Friendship
- Intimacy
- Family
According to Maslow, humans need to feel a sense of belonging and acceptance among their social groups, regardless whether these groups are large or small. For example, some large social groups may include clubs, co-workers, religious groups, professional organizations, sports teams, and gangs. Some examples of small social connections include family members, intimate partners, mentors, colleagues, and confidants. Humans need to love and be loved – both sexually and non-sexually – by others.[2] Many people become susceptible to loneliness, social anxiety, and clinical depression in the absence of this love or belonging element. This need for belonging may overcome the physiological and security needs, depending on the strength of the peer pressure.
Important stuff, here. We’ve seen this ball dropped too many times to ignore its impact on how well your buddy is going to do after he is injured. I would also add that one of the key elements to prevent is simple boredom. Shut up in a hospital room for 6-8 weeks, unable to move beyond your room, is a recipe for insanity.
Esteem
All humans have a need to feel respected; this includes the need to have self-esteem and self-respect. Esteem presents the typical human desire to be accepted and valued by others. Maslow noted two versions of esteem needs: a “lower” version and a “higher” version. The “lower” version of esteem is the need for respect from others. This may include a need for status, recognition, fame, prestige, and attention. The “higher” version manifests itself as the need for self-respect. For example, the person may have a need for strength, competence, mastery, self-confidence, independence, and freedom. This “higher” version takes precedence over the “lower” version because it relies on an inner competence established through experience. Deprivation of these needs may lead to an inferiority complex, weakness, and helplessness.
Self-actualization
Main article: Self-actualization“What a man can be, he must be.”[10] This quotation forms the basis of the perceived need for self-actualization. This level of need refers to what a person’s full potential is and the realization of that potential. Maslow describes this level as the desire to accomplish everything that one can, to become the most that one can be.[11] Individuals may perceive or focus on this need very specifically. For example, one individual may have the strong desire to become an ideal parent. In another, the desire may be expressed athletically. For others, it may be expressed in paintings, pictures, or inventions.[12] As previously mentioned, Maslow believed that to understand this level of need, the person must not only achieve the previous needs, but master them.
- Wound care: types of wounds, primary vs secondary intention, types of dressings vs types of wounds, how to make Dakins solution, improvising bandages, overall cleanliness, how to deal with infections, etc.
- Physical therapy (PT): generally considered to be gross motor tasks, such as how to walk again.
- Occupational therapy (OT): generally, fine motor tasks, such as how to use a fork or write again
- Ortho issues: how often to change a cast, how long should it stay on, when do you start moving it again, etc.
- Nutritional therapy (NT): how to fuel the healing process
- Covert aspects of the above
- General nursing issues: everything not listed above, such as bathroom issues, bathing, medications, emotional support, etc. Lots of stuff here.
- Logistics issues: get the stuff where it needs to go, and the “public health” issues surrounding it
- Training issues: teach your replacement, teach your covert nurses, etc.
- Medical texts to have available.
Thanks for stopping by.



A few years ago when I was recovering from lung surgery,due to pneumonia that turned into a bad lung infection-the day I got out of ICU-the doc told me to get my family and friends to bring me “real food” from home as I was more likely to eat it,and eat more of it than the hospital garbage,and that eating good food,getting enough rest,and getting up and moving were the things that would allow me to recover sooner.
I had lost a lot of weight-between 30-40#.
I got out of hospital in 3 weeks,with chest tubes and IV antibiotics,but still in half the time I was told it would take. The docs said it was due to the “real food”,and me doing all the PT I was told to do.
LikeLike
Sounds like you are pretty hard to kill Larry. Great story.
LikeLiked by 1 person
Pingback: Hogwarts: Convalescent Care In Grid-Down And Covert Environments: Part I – Introduction | Western Rifle Shooters Association·
As an experienced Internal Medicine physician and a few years as a Flight Surgeon w the USAF (CASF, C4), the thought of grid down medicine terrifies me. First, anyone’s ability to practice medicine will be markedly diminished without supplies (medications, sterile anything) that now magically appear, without XRay/CT/MR/US to ply my trade. I think the state of medicine will be reduced to that of the Civil War except with the understanding that bacteria are causing infections but without the ability to treat. Amputations will done as quickly as possible (no anesthetics) rather than painstaking internal or external fixation. “We’ll see if he makes it through the night” rather than transferring to an ICU setting.
For those that survive the golden hour will then face the “silver week” to see who dodges fatal infections and organ failure pretty much on their own without ventilators, IV anything, sterile anything.
Then the “brass” month(s) for the survivors – their convalescent care. This is where I think ‘something’ can be done, though difficult and time consuming, about as well as today. The same can be achieved in a grid down environment given enough resources – think of the volume of firewood needed just to heat enough water to wash sheets contaminated w stool or puss achieve semi-sterilty. You will need tribe.
We may soon return to an age where a simple splinter can cascade into death. Yes, there are ‘natural’ antibiotics for superficially infected wounds like garlic, sugar and honey. But there’s a reason why those little tubes of goop (neosporin and etc) relegated garlic, sugar and honey back to the kitchen. There’s a reason why the tombstones of graveyards pre-dating the antibiotic/modern medicine era are full children.
And yet prep I do. I really need to find some good quality hand saws and perhaps a drill.
LikeLike
Your fears are shared deeply. Watching the focused attacks on the pharmacies during the Baltimore riots really drove home how ugly things could get. Its bad enough not to have electricity. Adding to the mix roving packs of brigands that would happily destroy a field hospital and its patients to satiate their desires to get high makes for a very bad day.
Hope to see you on the sequential posts on this. We love hearing from other clinicians with their ideas and experiences with this stuff.
LikeLike
I completely left out security concerns – no matter who rolls you up and asks ‘whats in that bag’ – whether its a looter or a badge, you lose. Tunnel vision is dangerous.
In med school, we would ridicule previous generations of physicians who busily categorized symptom complexes into diagnosis (ie a named disease) but were powerless to treat them. A very snarky ‘wow, Dr. X, you got a disease named after you but couldn’t treat it worth a damn (not like us who can treat it)’. Arrogance!
Living in a state w legalized medical cannabis, I got over my stigma and began to look into the research and remain amazed. Enter ‘medical cannabis’ in the internal search engine of sciencedaily.com for a sampling. For those that can do so legally, having a cache of various strains will save lives. How else to treat seizures after big pharma collapses? Can’t get that knee replaced – a high CBD topical applied a few times a day may keep you walking once you go through your opiate Rx….
And might as well have some recreational strains – alcohol requires a surplus of foodstuffs (grapes, potatoes, grain etc) and manpower
LikeLike
In austere 3rd world medicine every attempt is sometimes made to salvage a limb even in the face of impending sepsis when the odds of survival as a amputee are low. After you recover him he may have to be able to still work for food every day. Limbless it may all be for naught.
LikeLike
looking forward to this series. It would seem that out of necessity it would be prudent to look into alternative ways to prevent infection and deal with some of the other issues – herbalism seems to fit the bill for a small chunk of these issues. Perhaps get in contact with Sam Coffman from the Human Path for a follow on series for herbal long term care and infection prevention.
I sure am glad for ERs and modern medicine, but knowing other options makes a lot of sense.
LikeLike
It is fairly easy to synthesize diethyl ether for at least crude anesthesia, http://breakingbad.wikia.com/wiki/Diethyl_ether. Ethanol can be distilled from most grain crops, sulfuric acid is available from old car batteries…
Other inhalation anesthetics like chloroform can also be sythesized from relatively common materials https://www.erowid.org/archive/rhodium/chemistry/chloroform.html
And surgery was done for a hundred years with such basic aids. No, it won’t be the same as today, but it will be possible to do good medicine.
Likewise, products can be sterilized using a pressure cooker as an autoclave, and if we can’t save everyone, we can at least save some or most.
For pharmaceuticals, especially antibiotics, chloramphenicol can also be made at home – not the best choice for most infections, but….something. If there is something you really, really need it is best to either stock a lot of it now so that it will last, or figure out a way to make it or do without.
Failure (defined as not attempting to save lives) is not an option for me.
LikeLike
“chloramphenicol can also be made at home” can you expound on this?
thanks
(As a work of caution to readers making diethyl ether is highly flammable. Do it outside with steam from a long hose as your off grid heat source, not a fire.)
LikeLike
We did it in Ochem lab in college….
https://www2.chemistry.msu.edu/faculty/wulff/myweb26/research/natural_products.htm
LikeLike
You guys OK? Part II?
LikeLike
So its been over a year since the last post and i still check back to see whats happening. Any chance you will be restarting the site?
LikeLike